Spring Research Roundtable Summary
Welcome to Science with Sandra!
This month I wanted to share a brief summary of the Spring edition of our Research Roundtable. It took place on Tuesday, April 23rd with the participation of two incredible guest speakers: Dr. Elizabeth Radford and Dr. Abraham Al-Ahmad.

The Research Roundtable was well attended with 35 participants from different places within the country and other countries around the world. We were grateful to have researchers as well as clinicians and parents participate in this meeting.
Our first speaker was Dr. Elizabeth Radford, who is an academic lecturer in Pediatric Neurology in the University of Cambridge. She is interested in researching the genetic and epigenetic factors controlling infant and child development and how changes in the developmental trajectory can lead to developmental disorders.
Dr. Radford shared her work in determining the functional implications of genetic variants in GLUT1 Deficiency.
Dr. Radford explained she is using a CRISPR-based saturation genome editing technique with the overall goal of improving developmental disorders diagnosis, including GLUT1 Deficiency. One of the reasons behind this project is that variant interpretation in developmental disorders is challenging because we still understand relatively little about our genetic code. When interpreting variants, we gather information from a variety of sources: for example, whether or not the variant has been seen in the healthy population; if the variant has been observed in patients with similar symptoms; or if the variant has occurred de novo. A De novo variant means that the variant or DNA change is seen for the first time in a person and has not been inherited from their parents.
Currently, there are in silico, or computer-based tools, available that aim to help with variant interpretation. However, experiments that directly test the function of genetic variants are scarce and are urgently needed at scale to help determine if variants of unknown significance (VUS) are disease-causing or not. The ability to accomplish this will make a huge impact on diagnosis. This is particularly urgent for conditions where there is an available treatment that could potentially help the patient, such as for GLUT1 Deficiency.
Dr. Radford explained that the technique she is using for this study is called Saturation Genome Editing or SGE. This is a technique that utilizes CRISPR/Cas9-stimulated homology-directed repair to introduce specified genetic variants into the gene in human cells grown in a dish. For this study she works with a cell line for which the SLC2A1 gene is essential. This means that if the cells do not have a working copy of the SLC2A1 gene, they will die. The SLC2A1 gene encodes for the GLUT1 protein. The use of the CRISPR/Cas9 technology allows to make cuts on the SLC2A1 gene, where then a DNA fragment with a specific variant is introduced. The goal of her study is to introduce every possible DNA variant on the SLC2A1 gene to study the functional effect of each of those variants.
Dr. Radford and her team have been able to generate over 4500 variants so far and have determined their functional effect. The results show defined groups of variants depending on the functional effect. By comparing her results for variants that are known to be pathogenic and benign, Dr. Radford can estimate the specificity and sensitivity of her data. The results indicate that SGE is a good test that will be informative for clinical data interpretation.
Her future goals include to complete the process of introducing and analyzing all possible single-nucleotide variants in the SLC2A1 gene. She would be interested in collaborating with other groups to use her model to test possible therapeutic compounds to determine their functional effect.
Our second guest speaker was Dr. Abraham Al-Ahmad. Dr. Al-Ahmad is an Assistant Professor of Pharmaceutical Sciences at Texas Tech University in Amarillo Texas. Dr. Al-Ahmad’s main research interest focuses on understanding the cellular and molecular mechanisms by which the disruption of the blood brain barrier occurs following ischemic stroke injury, amyloidopathies, and in GLUT1 Deficiency.
Dr. AL-Ahmad talked about his work on GLUT1 Deficiency-induced pluripotent stem cells (iPSCs).
Dr. Al-Ahmad began by describing the blood brain barrier (BBB), which is a tightly locked layer of cells that defend the brain from harmful substances, germs, and other things that could cause damage. This barrier is composed of endothelial cells, pericytes and astrocyte-end feet. He described how the GLUT1 transporter is expressed in red blood cells, endothelial cells and astrocytes. Glucose present in the blood can go into the brain through this transporter (see diagram below).
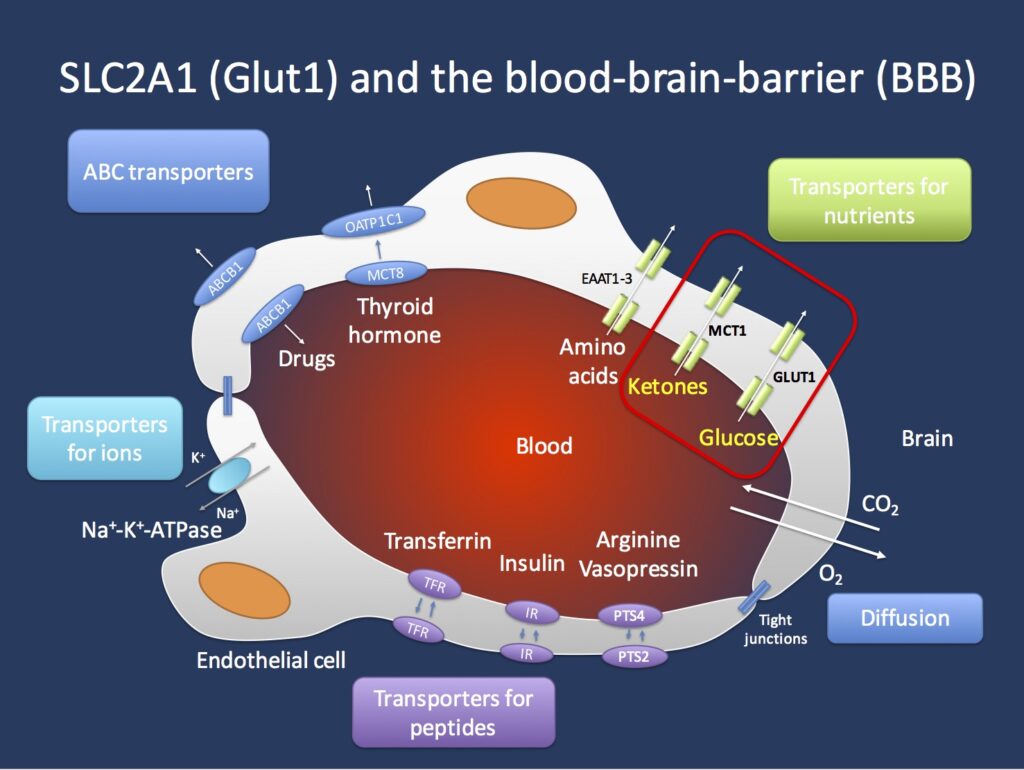
Source: Beyond the ion channel. The ILAE Genetics Commission blog.
To study the effects on GLUT1 Deficiency in the BBB, Dr. Al-Ahmad has generated two clones of induced pluripotent stem cells (iPSCs) deficient in GLUT1. The results show that these clones have a significantly lower expression of the GLUT1 protein. In addition, they have different effects in the protein structure and function, with one clone showing more severe effects than the other. Here you can find a link to the publication of the GLUT1 Deficient iPSCs and the characterization of the brain endothelial cells derived from them.
One of the goals of Dr. Al-Ahmad study was to differentiate these clones into cells of the neurovascular unit (NVU) to generate a GLUT1 deficient-BBB model in the future. Dr. Al-Ahmad and his team have been able to differentiate these GLUT1 deficient-iPSC clones into endothelial cells, astrocytes and neurons; these cells express proteins characteristic of each specific cell type and have their characteristic morphology.
With regards to the cells’ metabolism, Dr. Al-Ahmad and his team performed glucose uptake and ATP production tests. The results indicate that each clone uses different metabolic pathways to generate energy, and this changes depending on the cell type (endothelial, astrocyte or neuron). In general, all cells generated from the iPSC clones showed impaired glucose uptake. Interestingly, astrocytes and endothelial cells derived from the less severe clone showed unaffected ATP production. The reason behind it seems to be that this clone compensates the glucose absence by increasing the mitochondrial activity.
In conclusion, the disruption of the GLUT1 protein in these clones does not impact the iPSCs clones’ viability and ability to differentiate into different cell types such as endothelial, astrocytes and neurons. In addition, the glucose metabolism varies between cell types.
Dr. Al-Ahmad explained that among the future studies are to perform a transcriptome analysis of the differentiated cells to have a better understanding of the metabolic pathways impacted by the disruption of the GLUT1 protein in the BBB.
Please reach out if you have any questions or would like to get connected to Dr. Al-Ahmad or Dr. Radford. Thanks for reading!




